How Often Should Diabetics Screen for Neuropathy?
Patient's Query
I have diabetes and I keep hearing about ‘diabetic neuropathy’ (nerve damage).
How often should I get my nerves checked? Is it only when I get symptoms like burning feet, numbness, or tingling? Or should I screen even if I feel normal?”
Endocrinologist Answers

Neuropathy screening is not only for people with symptoms.
Many people have early nerve damage without realizing it, so regular screening helps catch problems early and prevent foot ulcers and infections.
The simple frequency rule.
- Type 2 diabetes
Screen for diabetic peripheral neuropathy starting at diagnosis, then at least once every year.
- Type 1 diabetes
Screen for neuropathy starting 5 years after diagnosis, then at least once every year.
This is the pattern recommended in major guidelines such as the American Diabetes Association (ADA) Standards of Care.
When screening should be MORE frequent.
If you have higher foot‑risk, such as:
- Loss of sensation.
- Poor blood flow.
- Foot deformity.
- Previous foot ulcer or amputation
Then screening should be more frequent than yearly.
The IWGDF (International Working Group on the Diabetic Foot) uses risk‑based intervals:
- Low risk (Risk 1) - loss of protective sensation (LOPS) or peripheral artery disease (PAD), but no deformity/ulcer history:
Screen every 6-12 months
- Moderate risk (Risk 2) - LOPS and PAD, or LOPS and deformity, or PAD and deformity:
Screen every 3-6 months.
- High risk (Risk 3) - LOPS or PAD plus previous ulcer, amputation, or end‑stage kidney disease:
Screen every 1-3 months
This more frequent follow‑up is to catch problems early and prevent new ulcers.
What “neuropathy screening” actually includes.
A proper clinic screening is quick and usually includes:
Symptom check:
Your doctor or nurse will ask about:
- Burning, tingling, or “pins and needles” in the feet.
- Numbness or “walking on cotton” feeling.
- Night pain in feet or legs.
- Reduced feeling of heat/cold.
These help pick up early nerve symptoms, but screening does not rely on symptoms alone.
Simple bedside tests:
Most standards recommend using a 10 g monofilament test plus at least one other test, such as:
- Vibration perception (e.g., 128 Hz tuning fork).
- Pinprick sensation.
- Temperature sensation.
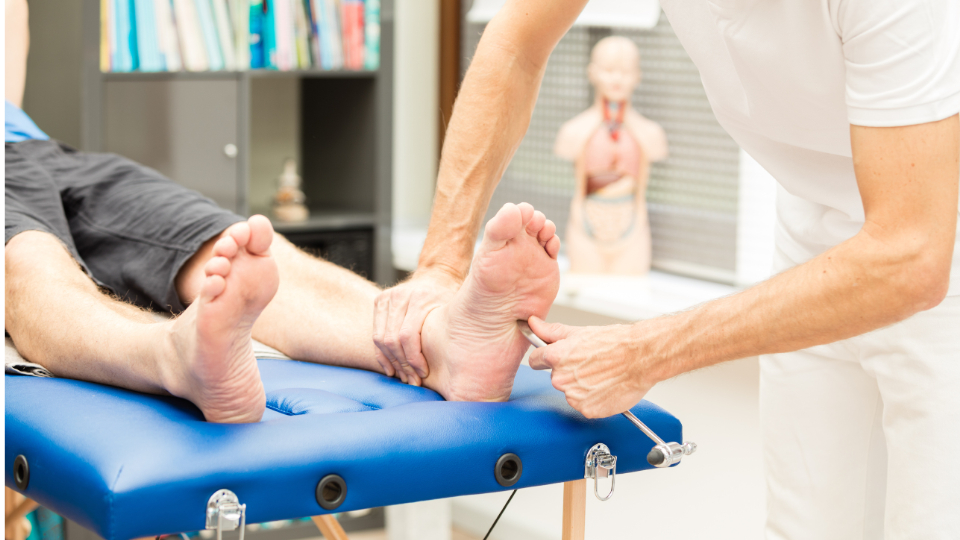
- Ankle reflexes.
The 10 g monofilament helps identify loss of protective sensation, which signals higher risk for foot ulcers. Adding another test improves accuracy.
Foot and circulation check:
Because nerve damage and poor blood flow is a dangerous combination, clinicians usually also check:
- Skin, nails, callus, cracks, deformities.
- Any redness, pre‑ulcer lesions, or existing ulcers.
- Foot pulses and signs of poor circulation.
This is part of a full diabetic foot exam, not just a monofilament tap.
If you are waiting for symptoms, don’t.
By the time numbness is obvious, protective sensation is often already reduced. That is exactly when:
- You may not feel cuts, burns, or stones in footwear.
- Ulcers, infections, and even gangrene can develop “silently”.
Because of this, guidelines recommend routine annual screening for everyone with diabetes (according to type and duration), even if you feel normal.
Quick “At Home” habits that reduce risk.
Even with yearly clinic screening, a daily self‑check is one of the strongest protections:
- Look at both feet every day (or ask a family member/help if you cannot see well): Cuts, cracks, redness, blisters, color changes
- Never walk barefoot, indoors or outdoors
- Check footwear for stones, rough seams, or foreign objects before wearing
- Moisturize dry skin on the feet (but not between toes) to avoid cracks
- Report any wound, redness, or blister that is not improving within 24-48 hours to your doctor or foot clinic
These habits plus regular clinic screening can prevent many serious complications.
References:
- https://diabetesjournals.org/care/article/47/Supplement_1/S231/153941/12-Retinopathy-Neuropathy-and-Foot-Care-Standards
- https://iwgdfguidelines.org/wp-content/uploads/2023/07/IWGDF-2023-02-Prevention-Guideline.pdf
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11040027/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8336435/
- https://drc.bmj.com/content/11/6/e003773
Disclaimer: The information provided in this Q&A is for educational purposes only and should not be considered as medical advice. Always consult with a qualified healthcare professional for personalized medical guidance and treatment recommendations.