Store Insulin Safely While Traveling in Hot Weather
Patient's Query
I’m traveling in a hot place. I’m scared my insulin will spoil. How do I store insulin safely during travel, in a hotel, or when I’m outdoors? What should I do if I don’t have a fridge all the time?
Endocrinologist Answers

The one rule that prevents most problems
Insulin must be protected from heat and from freezing. Heat can make insulin weaker. Freezing can permanently damage it.
Know the two “storage modes”
Unopened insulin
- Best kept refrigerated at 2°C to 8°C (36°F to 46°F).
- Never freeze. If it ever froze, do not use it. (Ref: official labels)
In-use insulin
- Many insulins can be kept at room temperature below 30°C (86°F) for a limited number of days.
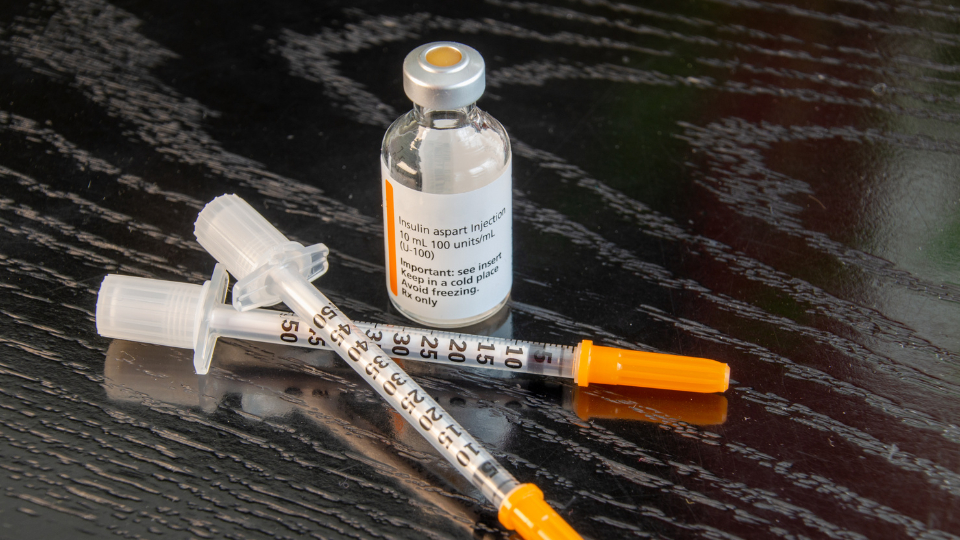
- Example: insulin aspart products commonly allow up to 28 days below 30°C (86°F). (Ref: NovoLog labeling)
- Some ultra-long acting insulins have longer “in-use” time at room temperature (example: insulin degludec allows longer in-use time, still with a max temperature limit). (Ref: Tresiba labeling)
Key point: “Room temperature allowed” does not mean “safe in a hot car or under direct sun.”
What to do during travel in hot climates
Best practical setup:
- Carry insulin in your hand baggage.
- Use an insulated pouch.
- Add a cool pack, but keep insulin separated from direct contact with the ice pack (wrap insulin in cloth). This avoids freezing.
- If you are outdoors for hours, consider an evaporative cooling pouch (works well in dry heat; less effective in very humid weather).
- Avoid direct sun: no window ledge, no dashboard, no backpack outer pocket.
Hotel, home stay, and office tips
- Use the refrigerator if available, but keep insulin away from the freezer compartment and away from the “cooling plate” where freezing can happen.
- If no fridge: keep insulin in the coolest indoor place, away from heat sources (kitchen, stove, hot water pipes).
- If you use a thermometer: try to keep the insulin storage area below 30°C (86°F) whenever possible (product-specific limits apply).
Red flags that suggest insulin may be damaged
Insulin damage is tricky because insulin may look normal and still lose strength. Still, these warning signs matter:
- Insulin was left in a hot car or direct sun for a long time.
- Insulin was frozen (or you suspect it froze).
- You suddenly see unexplained high sugars despite correct dosing, correct injection technique, and no infection or missed doses.
- The insulin looks abnormal (clumps, frosting, crystals, unusual cloudiness in an insulin that should be clear). Product inserts explain what “normal” should look like.
If sugars become unexpectedly high during travel and don’t respond to your usual correction plan, assume storage could be part of the problem and contact your clinician.
A simple travel checklist.
- Carry extra insulin and supplies for more days than planned.
- Carry a prescription or doctor note for airport security.
- Keep a backup method (syringes/pen needles), not just one device.
- Keep fast sugar for lows (glucose tablets).
- If you use CGM, carry spare sensors/charger as needed.
Common myths
- Myth: “If it looks fine, it’s fine.”
Truth: Heat damage may not change appearance. - Myth: “Ice directly touching the insulin keeps it safer.”
Truth: Direct ice contact can freeze insulin and ruin it. - Myth: “Any insulin can stay out in any heat.”
Truth: Temperature limits matter. Check your exact insulin’s label.
References:
Disclaimer: The information provided in this Q&A is for educational purposes only and should not be considered as medical advice. Always consult with a qualified healthcare professional for personalized medical guidance and treatment recommendations.