Frozen shoulder in diabetes: causes, stages, exercises, and recovery timeline
Patient's Query
I have diabetes and for the last few months I am unable to lift my hand above my shoulder. I cannot comb my hair properly, wear clothes comfortably, or reach overhead.
There is pain, especially at night, and stiffness keeps increasing. An orthopaedic doctor told me this is frozen shoulder and said it is common in diabetes, especially if sugars are not well controlled.
I am worried. Is this really because of diabetes? Will controlling my sugars reverse it? What exercises should I do, how long does recovery take, and will my shoulder ever become normal again?
Endocrinologist Answers

Yes, frozen shoulder is clearly linked to diabetes, and what you are experiencing is very typical.
Frozen shoulder, also called adhesive capsulitis, is not a muscle problem. It is a problem of the shoulder joint capsule, which becomes thick, tight, and fibrosed.
Why diabetes increases frozen shoulder risk
From both clinical experience and research evidence:
- Diabetes causes collagen glycation.
- This leads to fibrosis of the shoulder capsule.
- Inflammatory mediators and fibroblasts remain active longer.
- The capsule loses elasticity and movement becomes restricted.
People with diabetes develop frozen shoulder:
- More frequently.
- At a younger age.
- With more severe stiffness.
- With slower recovery compared to non-diabetics.
This is not because you “used your shoulder wrongly”. It is a metabolic effect.
The three stages of frozen shoulder
Based on current evidence and your uploaded reference, frozen shoulder progresses through overlapping stages:
1. Freezing stage
- Increasing pain, often worse at night.
- Gradual loss of movement.
- Inflammation dominates.
2. Frozen stage
- Pain may reduce.
- Stiffness is severe.
- Daily activities become difficult.
3. Thawing stage
- Pain settles.
- Movement slowly improves.
- Recovery phase.
In diabetes, symptoms may persist longer and overlap between stages.
Will sugar control cure frozen shoulder?
Sugar control does not instantly cure frozen shoulder.
But:
- Poor control worsens stiffness.
- Good control improves healing response.
- Better control prevents progression and recurrence.
Think of sugar control as removing fuel from the fire, not as an instant painkiller.
Treatment that actually works
1. Physiotherapy is the backbone
Medicines alone will not fix frozen shoulder.
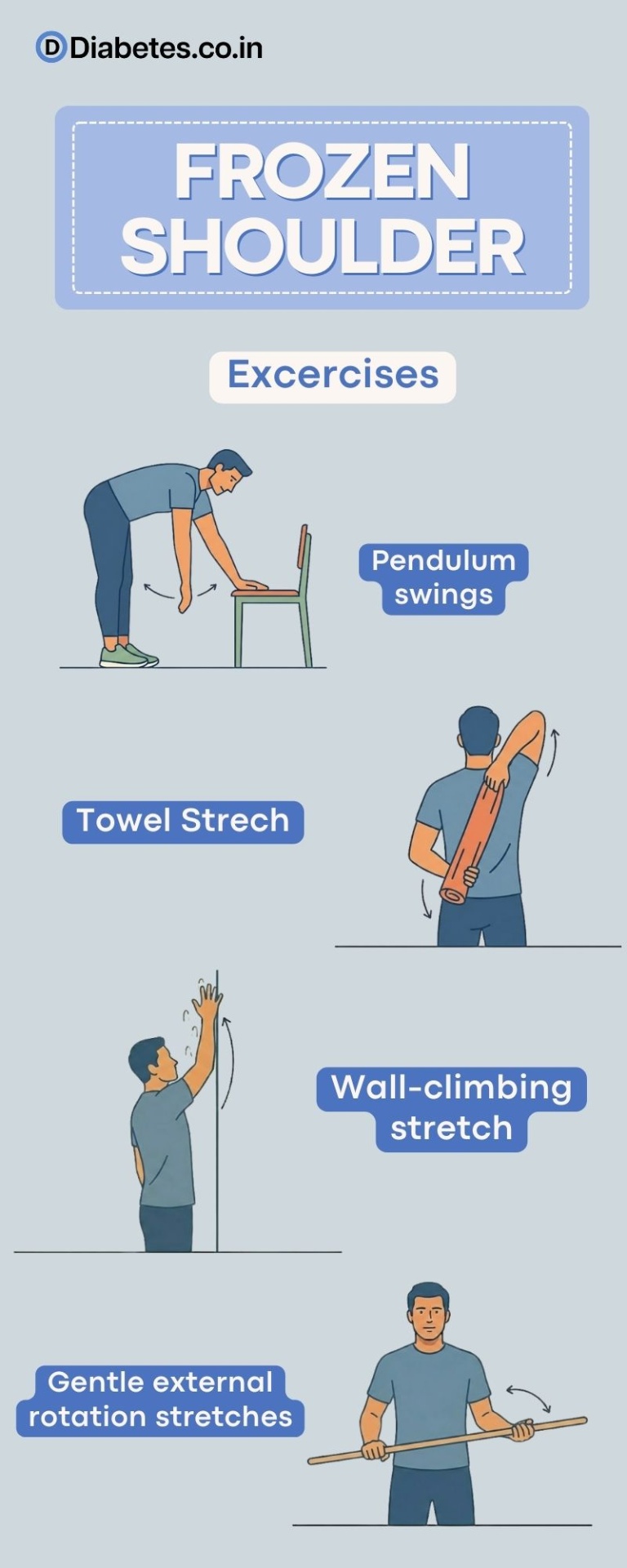
Key exercises:
- Pendulum swings.
- Wall-climbing stretch.
- Towel stretch behind the back.
- Gentle external rotation stretches.
Consistency matters more than intensity. Daily practice is essential.
2. Pain control to allow movement
Pain relief helps you perform exercises properly.
Options may include:
- Paracetamol or NSAIDs (if safe).
- Local steroid injection in selected cases.
Important diabetes note:
Steroid injections may temporarily raise sugars for a few days. Monitoring is needed.
3. What should be avoided
- Complete rest or immobilisation.
- Fear-based avoidance of movement.
- Aggressive exercises beyond pain limits.
Surgery and procedures
Most patients do not need surgery. Procedures like manipulation under anesthesia are reserved only for:
- Severe stiffness.
- Failure of prolonged conservative therapy.
Prognosis in diabetes
Be realistic but hopeful.
- Recovery usually takes 12-24 months.
- Diabetics recover more slowly than non-diabetics.
- Pain improves first, stiffness improves later.
- Mild residual stiffness may remain, but daily function usually returns.
One simple explanation I tell patients
“Frozen shoulder is slow, not dangerous. Consistency beats speed.”
References:
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4915459/
- The association between diabetes and frozen shoulder. J Bone Joint Surg. - Hand C
- https://pmc.ncbi.nlm.nih.gov/articles/PMC4363808/
- https://diabetesjournals.org/care/article/37/7/1863/37723/Musculoskeletal-Complications-in-Type-1-Diabetes
Disclaimer: The information provided in this Q&A is for educational purposes only and should not be considered as medical advice. Always consult with a qualified healthcare professional for personalized medical guidance and treatment recommendations.